
Due to maceration on the posterior lip of the cervix, true erosion often occurs. In addition to whites, in this case, the woman notes itching and burning in the vagina, in the area of the external genitals and perineum, due to their irritation by purulent secretions. 
The specific inflammatory process in gonorrhea in women most often involves the cervix. Gonorrheal cervicitis (endocervicitis).This sign is often regarded by a woman as a manifestation of nonspecific vaginitis or thrush, and therefore attempts are being made to treat the infection independently, erasing the true clinical picture. The classic signs of the disease are the appearance of abundant vaginal discharge of white or yellowish color with an unpleasant odor. Local manifestations depend on the predominant lesion of a particular organ, but gonorrhea in women often occurs in a mixed form. In almost half of infected women, gonorrhea has an asymptomatic or low-symptomatic course. The incubation period for lesions of the lower genitourinary tract is on average 5-10 days (with ascending, disseminated gonorrhea and estrogenital forms may increase). Symptoms of gonorrhea in women Gonorrhea of the lower genitourinary tract The course of gonorrhea in women can be uncomplicated and complicated. According to the localization principle, gonorrhea of the lower parts of the genitourinary tract ( urethritis, paraurethritis, vestibulitis, bartholinitis, cervicitis) and gonorrhea of the pelvic organs ( endometritis, salpingitis, adnexitis, pelvioperitonitis) are differentiated. There are genital and extragenital forms of gonorrhea in women. In the absence of specific local manifestations, but the release of the pathogen in the scrapings from the mucous membranes, they talk about latent infection, or gonococcus. Chronic infection, as a rule, is asymptomatic, with periodic exacerbations. Taking into account the severity of the symptoms, the fresh form may have an acute, subacute or torpid course. Classificationĭepending on the prescription of the disease, there are fresh (lasting up to 2 months) and chronic (lasting over 2 months) gonorrhea in women. The ascent of infection is facilitated by childbirth, intrauterine interventions (probing of the uterine cavity, abortion, RVV), menstruation, non-compliance with intimate hygiene. 
Household infection is extremely rare – mainly when a child is in close contact with a mother with gonorrhea (for example, in the case of using a shared bed, towels, hygiene items, etc.).įactors contributing to the high prevalence of gonorrhea among women are the low level of general culture, early onset of sexual activity, numerous sexual relationships, neglect of barrier methods of contraception and spermicidal agents during casual sexual intercourse, prostitution. The non-sexual path of infection can be realized during childbirth when the child passes through the birth canal. Often there is a multi-focal, multi-organ lesion. The predominant way of infection is sexual, infection is possible both with unprotected vaginal and oral-genital or anal-genital contact. Quite often, gonorrhea in women occurs in the form of a mixed infection: gonorrhea-chlamydia, gonorrhea-trichomonas, gonorrhea-mycoplasma, gonorrhea-candidiasis. Usually gonococci initiate a specific local inflammation, but when they get into the blood they can cause a disseminated gonococcal infection. Phagocytes are produced by polynuclear neutrophils, within which they retain viability and the ability to reproduce. With the help of surface proteins, gonococci attach to the cells of the cylindrical epithelium, causing their death and peeling. Gonococcus pathogenicity factors are: a capsule with antiphagocytic activity villi with which the bacterium attaches to the epithelium endotoxin secreted by the cell wall membrane proteins with pronounced antigenic properties. Inside the human body, the pathogen is highly resistant, it quickly dies in the external environment. The pathogen causing gonorrhea, Neisseria gonorrhoeae, is a gram-negative aerobic diplococcus having a bean-shaped form. A high degree of contagion, the appearance of strains of gonococcus resistant to known antibiotics, an adverse effect on reproductive function – these and other factors make the prevention of gonorrhea a priority task of venereology and gynecology. With a single unprotected sexual contact with a partner with gonorrhea, the risk of infection is 60-90%. Most cases of gonorrhea are diagnosed in women aged 15-29. In the structure of STIs, it ranks second in prevalence after chlamydia and is often detected simultaneously with it. 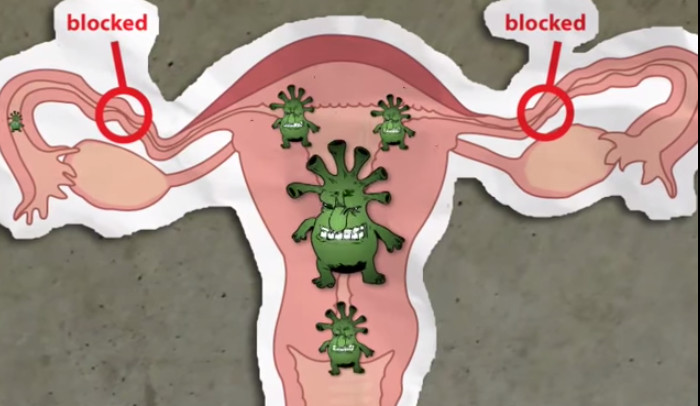
Gonorrhea in women is a venereal disease that can occur in urogenital (gonorrheal urethritis, cervicitis, bartholinitis) and extragenital forms (gonorrheal proctitis, stomatitis, pharyngitis, blennorrhea).
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
